Imagine a symphony orchestra where every musician plays their own sheet music, completely unaware of what the others are doing. The result would be chaos, not harmony. This is the reality of healthcare today—a fragmented system where specialists, primary care providers, and behavioral health professionals operate in silos, each with their own isolated view of a patient.
This silent crisis of disconnected care has real, quantifiable consequences:
- For providers: It leads to burnout, administrative overload, and the constant fear of missing a critical piece of information that could impact a patient’s health. Up to 48.2% of physicians reported experiencing at least one symptom of burnout as of 2024-2025
- For patients: It results in medical errors, redundant tests, conflicting medication plans, and a profound sense of frustration as they navigate a complex and confusing system. Between 250,000 and 400,000 deaths per year in the United States are attributed to medical errors, making it one of the top three leading causes of death, alongside heart disease and cancer

How disconnected care affects the provider?
From the provider’s point of view, this is what a typical day looks like without a collaborative care coordination:
- The EHR is a data graveyard: The electronic health record is often an incomplete snapshot. A provider’s EHR only contains the information they have personally documented, leaving them blind to what other specialists have prescribed or recommended.
- Communication is a game of telephone: The primary method of communication is often phone tag, faxes, or unsecured emails. It’s time-consuming, inefficient, and prone to errors.
- Administrative burden is overwhelming: Hours are spent chasing down lab results, calling other specialists for updates, and manually compiling a patient’s medical history. This isn’t patient care; it’s tiring administrative tasks.
- Patient outcomes are at risk: The lack of a shared, comprehensive view of the patient makes it difficult to make informed decisions. A medication conflict, a missed follow-up, or an undiagnosed mental health issue can easily slip through the cracks, leading to a costly readmission or a negative health outcome.
Care coordination isn’t optional anymore—it’s the backbone of quality care. But it only works when it’s connected, efficient, and built to handle every moving part. That’s where blueBriX makes a difference.
The blueBriX approach to care coordination: a step-by-step blueprint
The blueBriX platform transforms the outdated model into a seamless, intelligent workflow that supports true multidisciplinary care. Here is a step-by-step breakdown of how blueBriX powers this efficient, connected approach:
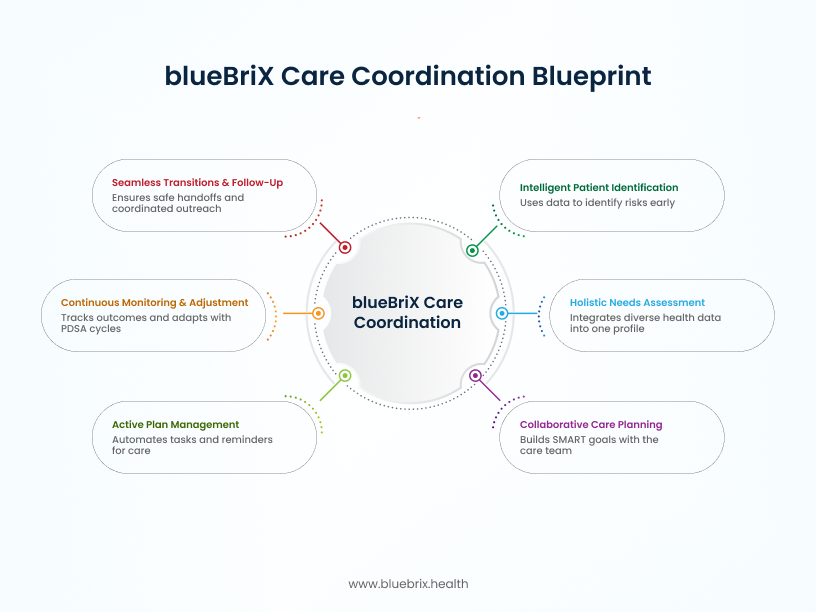
Step 1: Intelligent patient identification & risk stratification
Before a patient’s condition escalates, blueBriX is already at work. Our platform ingests and analyzes data from EHRs, claims, labs, and social determinants of health (SDoH) to spot risks early.
Predictive modeling automatically classifies patients into risk tiers (high, medium, low) and flags complex cases. For example, a patient with a new cardiology diagnosis, uncontrolled diabetes, and a history of insomnia is instantly identified as high priority.
- Behavioral health: Integrated screenings (PHQ-9, GAD-7, CAGE, MDQ) capture mental health concerns alongside physical conditions.
- Primary care: Care gaps surface automatically through integrated data, enabling proactive outreach.
- Specialty programs: From Framingham Risk Scores in cardiovascular care to identifying isolated seniors in preventive programs, the platform applies the right stratification method for each domain.
Step 2: Comprehensive, holistic needs assessment
Once a patient is flagged, blueBriX unifies physical, behavioral, functional, and social assessments into a single, accessible profile.
Instead of siloed evaluations by different providers, all inputs—from lab results to psychosocial assessments—are captured in one dashboard.
- Behavioral health: Tracks treatment goals, symptom scales, and social support systems.
- Chronic disease programs: Integrates HbA1c, BP, lipid profiles, and lifestyle data to guide intervention strategies.
- Cancer care: Facilitates multidisciplinary tumor board inputs, storing all staging and treatment decisions centrally.
Step 3: collaborative & patient-centered care plan development
The best care plans are built with the patient, and not just for them. The platform supports joint creation of SMART goals, assigns responsibilities, and keeps all team members—PCPs, specialists, behavioral health clinicians, and care coordinators—aligned.
- Dental care: Oral health goals can be integrated alongside systemic health goals.
- Cardiovascular care: Medication and lifestyle interventions are coordinated with mental health considerations to avoid drug interactions.
- Preventive programs: Care pathways incorporate community screenings and wellness check schedules.
Step 4: Active care plan management & execution
Care plans often fail in execution. blueBriX makes sure they don’t. Automated task assignments, appointment reminders, RPM integration, and real-time data tracking keep interventions on schedule.
- Behavioral health: Missed therapy sessions trigger alerts to care managers.
- Chronic care: RPM flags dangerous glucose spikes or BP readings before they lead to ER visits.
- Dental programs: CAD/CAM workflows and appointment recalls are integrated to maintain continuity.
Step 5: Continuous monitoring, evaluation, & adjustment
Care coordination is a continuous process. Real-time dashboards track progress against clinical markers and patient-reported outcomes. Built-in PDSA cycles enable quick adjustments.
- Diabetes programs: Continuous glucose monitoring data feeds into care reviews.
- Cancer care: Follow-up intervals are automated—three-month check-ins, then six-month, then annual—based on care stage.
- Preventive care: Community health metrics inform program refinements.
Step 6: Seamless transitions of care & follow-up
Handoffs are high-risk moments. When patients change settings—hospital to home, specialist to PCP—blueBriX generates and shares comprehensive summaries with every relevant provider.
- Cardiovascular programs: Discharge summaries are sent to both cardiologists and rehab specialists.
- Behavioral health: Relapse prevention and check-ins are built into the post-discharge workflow.
- Preventive programs: Patients receive reminders for screenings and wellness visits, closing the loop on long-term engagement.
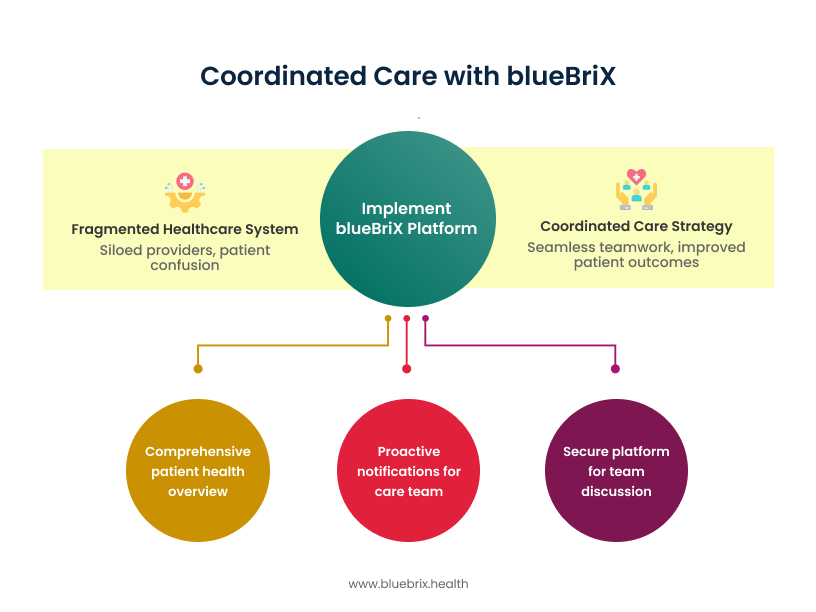
To see the real impact of integrated care coordination, let’s look at a common provider challenge—managing a patient with both psychiatric and cardiac conditions across multiple specialties.
Care coordination in action: a provider’s lens
Managing patients with multiple conditions is rarely about clinical expertise alone—it’s about communication. Take a common scenario: a 68-year-old with insomnia and a new CHF diagnosis. His psychiatrist, cardiologist, and PCP all want the best outcome—but without a shared system, coordination quickly unravels.
Without blueBriX: The cardiologist prescribes a beta-blocker, unaware it may worsen insomnia. The psychiatrist never hears about the new diagnosis. The PCP is left juggling faxes, trying to connect the dots. Providers are stuck in silos, and the patient is put at risk.
With blueBriX: A unified dashboard flags the drug interaction before it becomes a problem. The psychiatrist is automatically notified of the CHF diagnosis. All three providers co-create a shared care plan, exchange updates in real time, and track SMART goals together.
The difference: Providers spend less time chasing information and more time making confident, informed decisions. The result is safer care, smoother collaboration, and fewer gaps slipping through the cracks.





