The compliance tax is the hidden drain on modern healthcare margins. Every time a new mandate drops, whether it’s the Cures Act, TEFCA, or evolving AI privacy laws, most organizations pay a heavy price in downtime, developer fees, and lost productivity.
If your technology feels brittle, you aren’t just facing an IT problem; you are facing a business liability. Use this 5-point stress test to determine if your infrastructure is built for the future or stuck in the past.
1. The integration tax test
Can you connect to a new laboratory, a specialist’s registry, or a patient-monitoring app without paying your vendor a “connection fee” or waiting 6+ months for a custom build?
Why it matters: In a value-based care world, your margin depends on your ability to see the “whole patient.” If your EHR charges you a “toll” every time you want to talk to another system, they are effectively taxing your growth.
The impact of an agnostic system: When you use integration-agnostic infrastructure, adding a partner becomes a routine configuration task. Instead of waiting half a year to launch a new remote monitoring program, you can go live in weeks, capturing revenue while your competitors are still stuck in a vendor’s development queue.
2. The payer-pivot test
If you sign a new Value-Based Care (VBC) contract tomorrow, can your system adapt its reporting logic without a total database overhaul?
Why it matters: Payers are shifting requirements faster than ever. If your billing and clinical data are “hard-coded” together, a change in how Medicare wants data reported can force you to hire an army of manual data entry clerks just to get paid.
The impact of an agnostic system: A payer-agnostic core separates clinical documentation from the financial pipes. You gain revenue agility. You can accept complex, high-margin contracts because your tech can effortlessly generate the specific reporting those payers demand without interrupting the doctor’s workflow.
3. The AI safety-valve test
If your current AI transcription or diagnostic tool is flagged for a privacy violation, can you swap it for a different AI model (LLM) in a single afternoon?
Why it matters: AI is the “Wild West” of regulation. If your AI is “baked into” your EHR and that specific vendor fails a HIPAA audit or issued for data bias, your entire clinical engine stops.
The impact of an agnostic system: Being AI-agnostic means you aren’t “married” to one model. You treat AI like a utility. If a better, cheaper, or more compliant model (like a specialized medical LLM) hits the market, you simply plug it in. You get the cutting edge without the locked-in risk.
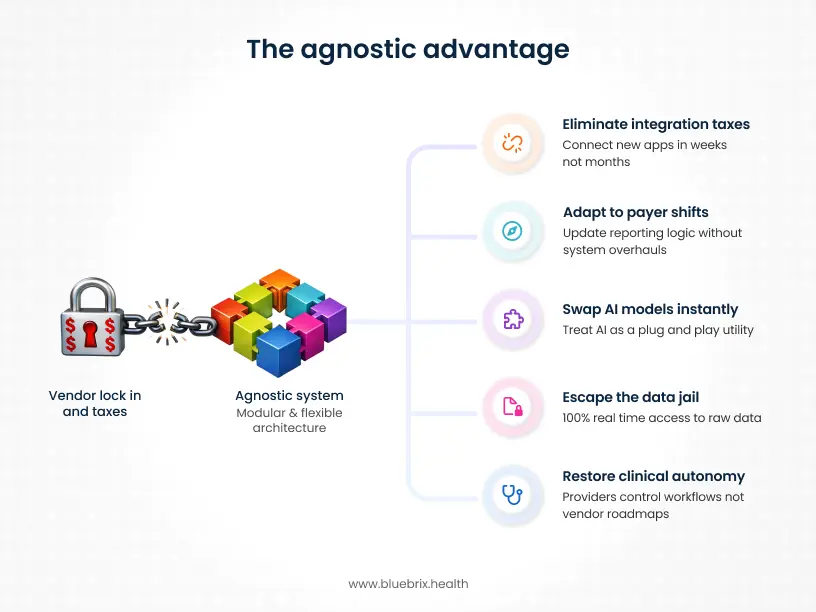
4. The data jail test
Do you have 100% real-time access to your raw clinical data, or must you “request an export” from your vendor to run your own analytics?
Why it matters: New information blocking mandates carry heavy federal penalties. If your vendor makes it difficult for you to move or analyze your data, your organization is the one legally and financially responsible.
The impact of an agnostic system: Data sovereignty means the data is in a universal format (model-agnostic) that you own. You can run real-time population health analytics to identify at-risk patients before they end up in the ER, drastically improving your performance in shared-savings models.
5. The clinical autonomy test
When clinical protocols change, can your Medical Director update the workflow in the system themselves, or are you stuck in your vendor’s development roadmap?
Why it matters: Clinical burnout is often software burnout. Doctors hate being forced into rigid, click-heavy workflows that don’t match how they actually practice medicine.
The impact of an agnostic system: A model-agnostic architecture wraps around your care delivery style. You can customize a Behavioral Health screen and a Cardiology screen within the same system. Your tech supports the doctor’s expertise rather than trying to replace it.
Ready to see a compliance-proof system in action?
In the 2026 healthcare landscape, the winners won’t be the ones with the most famous EHR brand names. They will be the ones with the most agile infrastructure—systems that can pivot as fast as the regulations do.Book a strategic consultation with blueBriX
Contact us



