Every year, preventable hospital readmissions cost the U.S. healthcare system over $17 billion. This is more than a financial drain; it’s a systemic failure with a human cost.
Consider John, a 72-year-old with heart failure. After a hospital stay, his cardiologist adjusts his medications. Without the care team knowing, his home monitor records a steady weight gain—a clear sign of fluid buildup. But because his data is siloed across the hospital, his primary care clinic, and the device app, no one sees the full picture. A week later, John is back in the ER with worsening symptoms that could have been prevented with a simple phone call.
John’s case highlights a critical problem: patient data is scattered across “data islands.” Electronic health records (EHRs), pharmacies, specialty clinics, and personal health devices rarely communicate effectively. This forces clinicians into a reactive cycle, where they are left to manage emergencies instead of preventing them.
Traditional healthcare data standards, like C-CDA, have long been used to share patient summaries. However, they package information into large, static documents—inefficient for real-time analysis. Pulling a single, critical data point, such as “weight gain in the last 7 days,” from a 30-page document is neither efficient nor predictive.
This is where FHIR (Fast Healthcare Interoperability Resources) represents a step-change.
What is FHIR and how does it unlock healthcare data?
FHIR is a modern data standard that breaks healthcare information into modular, queryable “resources” (e.g., Medications, Allergies, Observations). Unlike static documents, FHIR allows for granular, real-time data exchange. This means John’s weight readings, medication changes, and follow-up schedule can flow instantly to his care team.
How does FHIR provide a strategic foundation for digital health?
- Interoperability by design: FHIR uses a uniform set of structured data formats and accessible APIs, shifting health data from proprietary formats to open, consistent exchanges.
- Real-Time Data for analytics: FHIR data can be flattened and transformed into analytics-ready structures (like SQL-friendly tables), making it easy for business intelligence tools and AI models to consume and analyze.
- Improved data quality: FHIR platforms can validate incoming data to ensure accuracy and compliance with standards like SNOMED CT and ICD-10, building trust in the data used for care, reporting, and research.

How does AI create a predictive healthcare model combined with FHIR?
The true power of a predictive healthcare model lies in the collaboration between FHIR and AI, but it’s a journey that involves more than just a direct connection. While FHIR provides the universal language for data, AI provides the intelligence to turn that data into foresight. Data on its own is historical; it tells you where a patient has been. AI processes that information to forecast future outcomes.
This process transforms raw information into actionable intelligence, but it happens in two distinct steps that rely on a crucial intermediary layer.
Step 1: The FHIR foundation—creating a unified and structured data model
Before any predictive analysis can happen, an AI model needs a comprehensive and clean dataset. This is where FHIR is indispensable. It acts as the “universal translator” for all healthcare data sources, pulling in information that was previously trapped in disparate systems.
- From data islands to a unified lake: FHIR’s API-based architecture allows a system to connect to diverse data sources—including EHRs, lab results, pharmacy databases, and even mobile health apps. Importantly, a separate layer of software is often needed to handle data from sources like remote patient monitoring devices. This gateway or intermediary software pulls raw data from the device and structures it into the FHIR format, making it accessible to the broader healthcare system. This standardization is what creates a single, comprehensive “data lake” for each patient.
- Structured for AI: AI models, particularly those for predictive tasks, thrive on structured data. Instead of sifting through free-text doctor’s notes or complex, nested C-CDA documents, FHIR provides data in an organized, tagged format. This structure is the starting point, but it’s not the final step. The data in FHIR format must be further transformed and broken down into the specific, pre-processed format that a machine learning model needs for training. This intermediary step ensures the data is in the most optimal form for the AI to “learn” from.
Step 2: The AI engine—from data to foresight
With a unified and structured dataset provided by FHIR, the AI model can begin its work. It’s no longer just a simple algorithm; it’s a sophisticated “predictive engine” that analyzes a wide range of variables simultaneously.
- Holistic risk assessment: The AI model analyzes a patient’s FHIR-compliant data in a holistic way, looking for patterns that a human clinician might not have the time or capacity to identify. This analysis goes beyond simple lab results and diagnoses. It includes:
- Clinical data: Diagnoses, lab results, vital signs (e.g., heart rate, blood pressure, weight), and medication history.
- Unstructured data: Natural Language Processing (NLP) is used to extract key information from unstructured data like a doctor’s notes or discharge summaries and turn it into structured FHIR resources for analysis.
- Social determinants of health (SDOH): Critically, the model can incorporate non-clinical data like a patient’s living situation, access to transportation, or food security. This is often the most important predictor of a patient’s health trajectory.
- Generating actionable risk scores: By sifting through all these complex data points, the AI can generate a real-time, actionable risk score for a patient. For example, a patient with heart failure might have a high-risk score because the model has identified:
- A pattern of weight gain (from a wearable device via FHIR).
- A new prescription (from the pharmacy record via FHIR).
- A lack of social support (from the SDOH data).
- A missed follow-up appointment (from the EHR via FHIR).
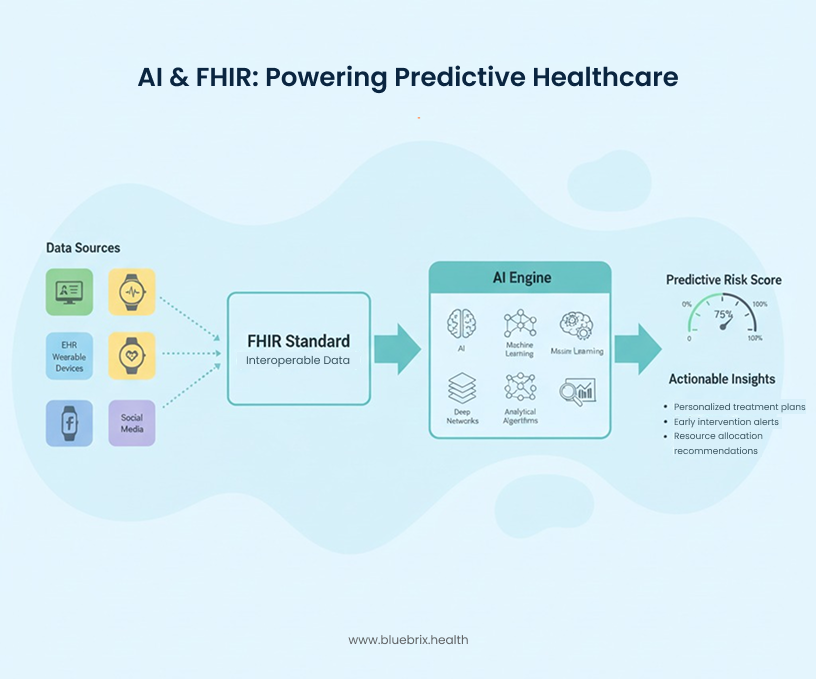
This real-time risk score identifies exactly which patients are most likely to miss a critical follow-up, be readmitted, or suffer an adverse event. It empowers clinicians with the information they need to intervene proactively, before a manageable trend becomes a medical crisis. In essence, the combination of FHIR and AI transforms healthcare from a reactive system to a truly predictive one.
The power of FHIR + AI: 4 key benefits
The synergy between FHIR and AI drives a proactive, predictive healthcare model. This powerful combination allows healthcare organizations to:
- Reduce readmission penalties and costs: By identifying high-risk patients at discharge, an FHIR + AI system enables targeted, proactive interventions. Preventing a single readmission can save thousands of dollars and help a hospital avoid penalties under the CMS Hospital Readmission Reduction Program (HRRP).
- Optimize resource allocation: Predictive analytics can forecast patient admissions and discharges with a high degree of accuracy. This data-driven insight allows administrators to optimize staffing, manage bed availability, and streamline surgical schedules, reducing operational costs and improving the patient experience.
- Improve revenue cycle and value-based care: In a “value-based care” model, reimbursement is tied to patient outcomes. An FHIR + AI system helps hospitals improve key quality metrics by proactively preventing readmissions and closing gaps in care, leading to better reimbursement rates and more favorable contracts.
- Enhance patient loyalty and engagement: A proactive FHIR + AI system fosters a positive patient experience by providing personalized reminders and support. This continuous engagement builds trust and transforms patients into active partners in their own health, boosting satisfaction and loyalty.
The human impact: empowering patients and clinicians
Beyond the financial and operational benefits, the synergy of FHIR + AI transforms the human experience of health. It redefines the roles of both patients and clinicians, fostering a system that is not only more efficient but also more empathetic and effective.
For clinicians: an intelligent teammate, not a replacement
A common misconception is that AI is here to replace human expertise. In reality, AI acts as an intelligent co-pilot, a powerful teammate that automates administrative burdens and augments clinical judgment. The modern clinician’s day is often bogged down by a relentless stream of “invisible work”: sifting through disparate patient charts, manually documenting vitals, and triaging an endless queue of messages and alerts. This cognitive load and administrative burden are primary drivers of burnout.
An FHIR + AI system fundamentally changes this reality.
- A unified, comprehensive view: By providing a single, comprehensive patient record—seamlessly compiled from all data sources via FHIR—the system eliminates the need for clinicians to hunt for data across siloed platforms. A doctor can walk into an exam room with a 360-degree view of the patient’s health, from recent lab results to medication adherence from a wearable device.
- Predictive workflows: The system uses predictive analytics to highlight the patients who need the most urgent attention. Instead of a doctor or nurse having to manually review every single patient on their list, the system can flag a handful of high-risk individuals—for example, a patient with a complex chronic condition who has missed two medication doses and shows early warning signs in their vitals. This allows clinicians to prioritize their day, reducing cognitive load and freeing up invaluable time.
- Empowering, not deciding: The AI doesn’t make the decision for the clinician; it simply equips them with the most relevant, real-time insights to make a better-informed decision, faster. This frees clinicians from routine, tedious tasks and allows them to focus on the human connection—the compassionate, empathetic care that algorithms can never replicate.
For patients: a “personal GPS” for health
For many patients, navigating the healthcare system can feel like driving through a dense fog without a map. Discharge instructions are often complex, follow-up appointments get forgotten, and the sense of being on one’s own is all too common. An FHIR + AI system changes this from a reactive, daunting journey to a proactive, guided one. It becomes the patient’s “personal GPS for health.”
- Proactive, personalized guidance: The system uses AI to understand each patient’s unique needs and deliver personalized guidance directly to them. Imagine a patient like John, who has a new, complex medication schedule. His “GPS” doesn’t just send a generic reminder; it triggers a personalized alert on his phone with a simplified checklist, or a text message to a family caregiver, ensuring everyone is on the same page.
- Continuous, real-time support: If the system detects a potential risk—like a missed medication dose or an abnormal reading from a remote monitoring device—it flags it. This allows a care coordinator to reach out with a quick, empathetic phone call. This proactive, continuous support gives patients a sense of security and control, transforming a daunting experience into a collaborative partnership for better health.
How does blueBriX deliver this solution?
The vision of a proactive healthcare system is compelling, but the path to get there can seem daunting. blueBriX provides the platform that turns this framework into a tangible, positive impact. We understand the complexities of data integration, the ethical implementation of AI, and the need for seamless clinical workflows.
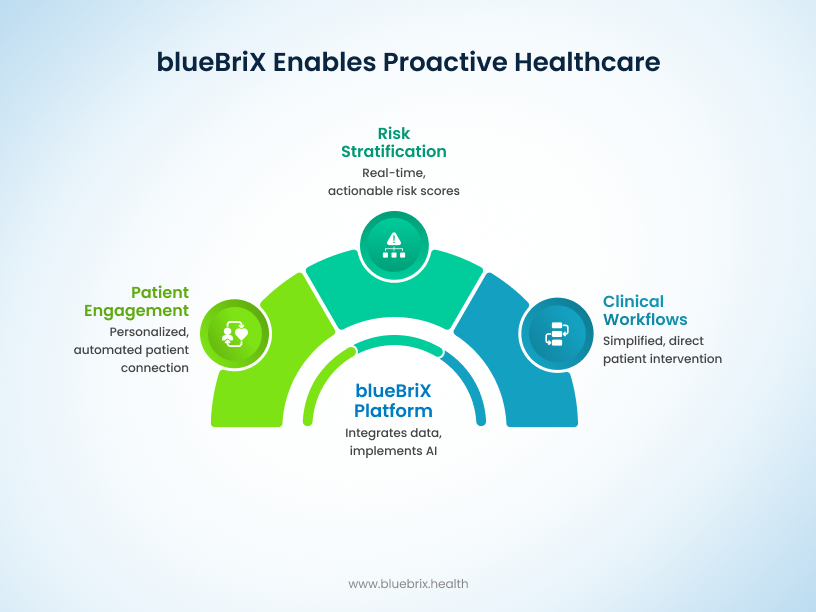
- Intelligent patient engagement: We use AI to create personalized and automated engagement strategies, ensuring no patient falls through the cracks. From sending medication reminders to delivering educational content, our system keeps patients connected to their care team, even after they leave the hospital.
- Predictive risk stratification: Our platform seamlessly ingests FHIR-standardized data from all your sources—EHRs, wearables, labs, and more. This unified data then feeds our sophisticated AI models, which generate real-time, actionable risk scores. This means your care coordinators and clinicians aren’t just looking at historical data; they are seeing a predictive forecast that highlights who needs their attention most, right now.
- Actionable clinical workflows: We believe technology should simplify, not complicate. Our insights are delivered directly into your existing clinical workflows, pushing alerts and notifications to the right team members at the right time. This removes the administrative burden of searching for information and allows your staff to focus on direct patient intervention, making proactive care a seamless part of their daily routine.
With blueBriX, you’re not just adopting technology; you’re gaining a partner with the expertise to navigate the complexities of this transition and transform your organization from a reactive provider into a proactive leader.
Building a responsible future with FHIR and AI: a trust framework
The true innovation of FHIR and AI is not just in their potential to transform health outcomes, but in our commitment to implementing them responsibly. A responsible approach requires more than checking boxes for compliance; it requires a proactive commitment to a trust framework built on three essential pillars.
Pillar 1: privacy and security by design
The foundation of any health solution is trust, and in the digital age, that trust is built on a non-negotiable commitment to data privacy and security. Instead of an afterthought, these principles must be foundational to the system’s architecture.
- Beyond compliance: Adhering to regulations like HIPAA and GDPR is the baseline. A truly responsible framework goes further by implementing robust, layered security. This means strong access controls, multi-factor authentication, and comprehensive audit trails that track every single data interaction.
- Data de-identification: A key strategy is to de-identify patient data wherever possible, ensuring that sensitive information is only accessible to those who absolutely need it for care. By securing data both at rest and in transit through encryption, we empower patients with control and give them confidence that their most personal information is safe.
Pillar 2: ethical AI and bias mitigation
AI models are only as effective as the data they are trained on. Without a deliberate focus on fairness, algorithms can inadvertently perpetuate and even amplify existing systemic biases, leading to unequal care. A responsible approach actively mitigates this risk.
- Diverse data, fair outcomes: The first step is using diverse and representative datasets that accurately reflect the entire patient population, not just a single demographic. This ensures the AI model is equally effective in diagnosing and predicting risk for all communities.
- Explainable AI (XAI): A trustworthy AI is not a “black box” that operates without scrutiny. We use Explainable AI (XAI) to make the algorithm’s decision-making process transparent to clinicians. This allows a doctor to understand not just what the AI is recommending, but why, which is essential for validating its logic and building trust in its recommendations.

Pillar 3: The indispensable role of human oversight
Even the most advanced AI is only a tool. The final pillar of our trust framework is recognizing that AI in healthcare is a powerful co-pilot, not an autonomous pilot.
- Augmenting, not replacing, clinicians: An AI model can process millions of data points, but it cannot replicate a clinician’s ability to show empathy, understand context, or use critical judgment. A doctor can interpret an AI alert in the context of a patient’s emotional state, their family situation, or their personal preferences, making a decision that is both clinically sound and deeply compassionate.
- Final accountability: The legal and ethical responsibility for patient care always rests with the human provider. Our system is designed to empower clinicians with insights, but the final decision to act—or not to act—remains in their hands. This human-in-the-loop model ensures that technology serves the patient and clinician, reinforcing that the human element is at the very heart of healthcare.




