Accurate and reliable assessments are the bedrock of any effective treatment. They guide diagnoses, shape interventions, and track patient progress, ultimately impacting well-being. Yet, a silent struggle often undermines this critical foundation: the inherent inconsistencies in manual assessment scoring. Imagine the ripple effect of a misdiagnosis stemming from a subjective score, or a treatment plan derailed by varying interpretations of a patient’s progress. These inconsistencies aren’t just minor inconveniences; they can lead to misdirected care, erode patient trust, and hinder the very outcomes we strive for.
How to improve behavioral health scoring with automation?
Behavioral health assessments are usually scored manually by clinicians. But factors like rater fatigue, unconscious bias, differing interpretations of scoring rubrics, or even simple calculation errors can compromise consistency. This makes it difficult to compare results across different clinicians, time points, or even patient populations, thereby hindering effective care management and research.

Enter automated scoring. By leveraging intelligent technology, behavioral health providers can overcome these challenges, ushering in an era of unprecedented assessment consistency. Let’s explore three significant ways automated scoring achieves this.
Way 1: eliminating rater bias and subjectivity

One of the most significant advantages of automated scoring is its ability to remove the subjective human element from the evaluation process. Human beings, by nature, are subject to biases. In the context of assessment scoring, these can manifest in various forms:
- Halo/horn effect: A general positive or negative impression of an individual influencing scores on specific items.
- Leniency/strictness bias: Some raters may consistently score more leniently or strictly than others.
- Fatigue: Scoring numerous assessments, especially complex ones, can lead to decreased attention to detail and inconsistent application of rules.
- Cognitive load: The mental effort required for complex scoring can lead to shortcuts or errors.
These subtle, often unconscious, biases can skew results, making comparisons between individuals or over time less reliable. Automated scoring systems operate on pre-programmed algorithms and precise rules. They don’t have opinions, emotions, or good/bad days. Every input is processed through the exact same logic, every single time. If a specific response triggers a specific score according to the programmed criteria, that score is assigned, without deviation.
This means:
- No two identical responses will ever receive different scores due to rater mood or interpretation.
- Scoring remains consistent whether it’s 9 AM on Monday or 5 PM on Friday.
- The system applies the exact same “lens” to every assessment, ensuring true objectivity.
Way 2: standardizing scoring rules and application

Beyond bias, automated scoring ensures that the rules themselves are applied with extreme precision. Behavioral health assessments often involve complex scoring methodologies. This can include:
- Weighted items: Different questions carrying different levels of importance.
- Subscale calculations: Aggregating scores from specific sets of questions to form distinct clinical constructs (e.g., depression, anxiety, trauma).
- Branching logic: Where a patient’s answer to one question determines which subsequent questions they see.
- Norm-referenced comparisons: Comparing an individual’s score to a large, representative sample.
Manually applying these intricate rules, especially across a high volume of assessments, is highly prone to error. Automated systems are designed to flawlessly execute these complex rules. Once programmed correctly, they will:
- Perform calculations instantly and accurately: Eliminating mathematical errors.
- Apply branching logic precisely: Ensuring patients only answer relevant questions.
- Process weighting and subscale aggregations flawlessly: Leading to accurate derived scores.
- Generate norm-referenced comparisons consistently: Providing reliable benchmarks.
This meticulous application of rules guarantees that the assessment results are free from subjective bias and unintentional human errors.
Way 3: increasing efficiency for scalability and frequent monitoring

The third major benefit of automated scoring is its unparalleled efficiency, which has profound implications for consistency and the overall quality of care. As caseloads grow, or as organizations seek to implement more comprehensive (and often longer) assessments, the burden on clinicians to score them accurately and promptly becomes immense. This pressure can lead to rushed scoring, which again compromises consistency.
Automated scoring systems can process vast numbers of assessments in mere moments. This speed means:
- No backlog: Assessments are scored immediately upon completion.
- Reduced clinician burden: Freeing up valuable clinical time that can be redirected to direct patient care or other critical tasks.
- Ability to use more detailed instruments: Without the scoring bottleneck, organizations can deploy more nuanced and informative assessments.
This efficiency ensures that regardless of the volume, every assessment receives the same high-quality, consistent scoring treatment. If you’re thinking scoring is anyway done by clinicians whether automated or manual, read on to understand how automated scoring can be the game-changer!
How accurate assessments help better outcomes?
Imagine a patient receiving vastly different scores on the same anxiety questionnaire depending on who scores it, or when it’s scored. Such inconsistencies can lead to misdiagnoses, inappropriate treatment plans, and a loss of trust in the healthcare system. High assessment consistency—meaning the evaluation yields similar results under similar conditions, regardless of external factors—is important. It underpins clinical validity, supports evidence-based practice, and ensures equitable care for all.
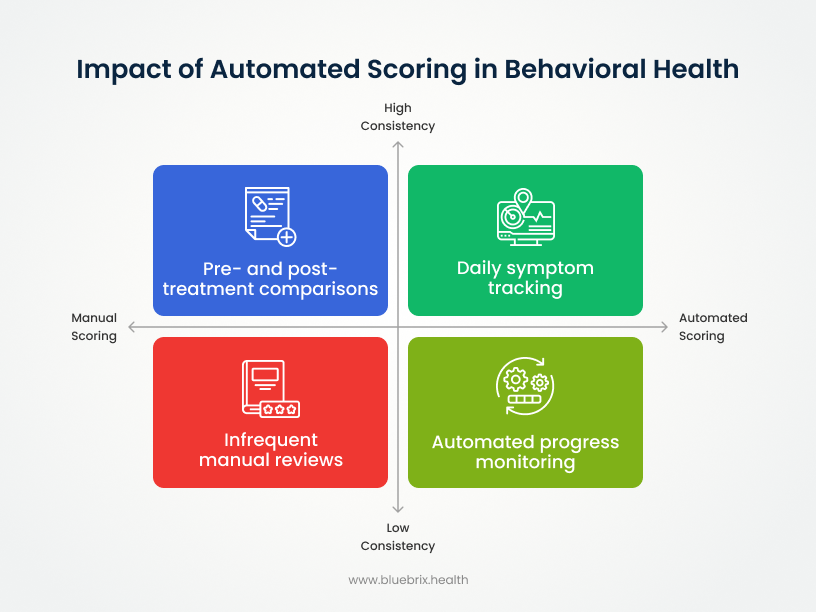
So, why are these assessments so vital? Let’s explore the key reasons:
1. Accurate diagnoses
Imagine trying to fix a complex machine without knowing what’s truly broken. That’s the challenge clinicians face without reliable assessments. Many behavioral health conditions, like depression and anxiety, can share overlapping symptoms. Reliable assessments are like sophisticated filters, helping clinicians distinguish between these conditions and arrive at a precise diagnosis. This means less “trial and error” and more direct, effective care.
2. Better outcomes
Treatment isn’t a static process; it’s a dynamic journey. Reliable assessments ensure this journey is effective and responsive. With accurate and up-to-date information from reliable tools, treatment plans become truly individualized. They reflect the patient’s current symptoms, their severity, and their progress, ensuring the care is always relevant. This vital feedback loop enables them to adjust interventions as needed, celebrate successes, and demonstrate the real impact of treatment.
3. Promotes patient well-being
At its heart, behavioral health is about enhancing patient safety and overall well-being. Reliable assessments are critical in achieving this. Reliable screening tools can identify mental health issues in their early stages. Without reliable tools, there’s a significant risk of misdiagnosis and inappropriate treatment. Such missteps can worsen symptoms and negatively impact a patient’s overall functioning and quality of life.
4. Fosters consistency
Imagine a world where different clinicians or clinics use entirely different methods to understand the same condition. It would be chaotic and hinder effective care. Standardized and reliable tools create uniformity across different clinicians, locations, and even over time. This ensures continuity of care, making it easier for patients to transition between providers or settings without losing valuable insights. This means when changes do appear in assessment results, clinicians can be confident that these reflect genuine variations in the patient’s status, not inconsistencies in the assessment tool itself.