Healthcare systems are facing unprecedented pressure due to staffing shortages, administrative overload, and increasing patient demands, revealing the unsustainability of traditional care models. While digitization has been a step forward, intelligent automation is the true solution. Virtual healthcare assistants are emerging as scalable and tireless digital partners, poised to support both patients and providers.
Let’s be clear: virtual medical assistants are not just chatbots
It’s a common misconception that virtual medical assistants are just fancy chatbots answering FAQs. Today’s virtual assistants are designed to understand context, personalize responses, and handle complex tasks. From managing appointments and medication reminders to guiding patients through recovery plans, these assistants can manage appointments, send medication reminders, and even guide patients through complex recovery plans.
Where they’re already proving themselves
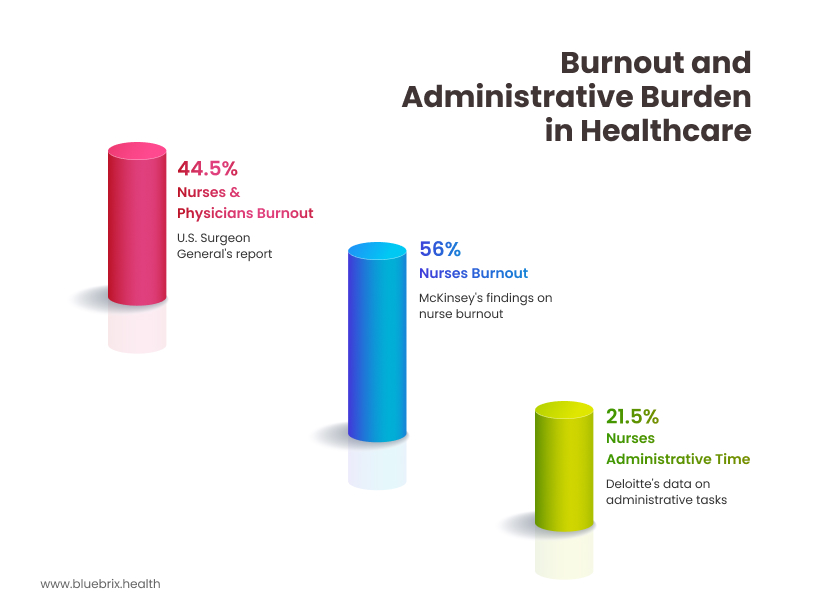
According to the U.S. Surgeon General (2022), 35–54% of nurses and physicians report symptoms of burnout. McKinsey (2023) found that 56% of nurses cite burnout directly, with administrative tasks being a top contributor. Deloitte (2024) reports that 15–28% of nurses’ time is spent on low-value administrative work—tasks that virtual assistants can help automate.
Across various healthcare settings, virtual medical assistants are already delivering tangible results:
- Post-visit follow-ups: Automating check-ins after discharge, helping reduce readmissions and ensuring patients adhere to care plans.
- Chronic care management: Offering daily health tracking, medication reminders, and timely prompts for patients managing conditions like diabetes and hypertension.
- Patient education: Delivering personalized guidance, procedural explanations, and medication instructions in simple, accessible language—available 24/7
The result? Higher patient engagement, lower no-show rates, and measurable relief for clinical and administrative staff.
But virtual healthcare assistants aren’t limited to basic automation—they are increasingly handling complex, multi-touchpoint workflows:
- Pre-surgical preparation: Guiding patients through pre-op instructions, forms, reminders, and scheduling lab work.
- Behavioral health support: Offering mental health assessments and directing patients to the right level of care.
- Insurance navigation: Answering benefits-related queries, estimating costs, and managing eligibility checks.
- Multilingual patient support: Enhancing accessibility through culturally sensitive, language-specific interactions.
- Care coordination for comorbid conditions: Keeping different specialists’ instructions aligned and patients informed.
These capabilities signal a shift from reactive tools to proactive, context-aware digital companions—seamlessly woven into the continuum of care.
And the possibilities ahead are even more transformative:
- Automated care orchestration: Coordinating post-discharge instructions, follow-ups, and home health referrals—all documented into the EHR.
- Predictive intervention alerts: Flagging deviations in chronic condition trends before they escalate.
- Always-on behavioral health check-ins: Helping support mental wellness between clinical visits.
- Smart referral and paperwork management: Assisting patients in locating in-network providers and completing pre-visit tasks.
- Targeted population outreach: Powering personalized campaigns for immunizations, screenings, and annual wellness visits.
Virtual medical assistants are rapidly becoming the connective tissue of modern healthcare—bridging patients, providers, and systems through intelligent, compassionate automation.
Why decision-makers can’t afford to wait
Consumer demand is shifting too. The CDC (2023) found that 41.5% of adults used the Internet to communicate with a doctor’s office. Deloitte (2024) reports that 24% of patients would switch providers just to gain access to better virtual healthcare options. Satisfaction with virtual visits is also high—over half of patients who’ve had one said they were “very satisfied.”
Healthcare delivery is evolving faster than ever—and standing still means falling behind. The administrative burden is growing, staff shortages aren’t going away, and patients expect responsive, digital-first experiences. Virtual medical assistants present a practical and scalable answer to this pressure.
What makes them truly compelling is their ability to adapt across workflows:
- They scale easily, supporting multiple departments or even entire care systems.
- They work with existing systems, reducing the need for costly overhauls.
- They offer transparency, with dashboards that show how patients are engaging.
- And they’re designed with healthcare privacy and security in mind from day one.
These aren’t futuristic tools—they’re here now, helping organizations run leaner, communicate better, and care more consistently. For leadership teams weighing the next big step, virtual medical assistants aren’t just an option. They’re an opportunity not to miss.
The real value: not replacing care, but reinforcing it
Evidence shows these assistants drive results. According to the American Journal of Preventive Medicine (2024), telehealth appointments had a 12% no-show rate compared to 25% for in-person visits. Deloitte (2024) estimates that automating front-desk workflows can save 700–870 staff hours per year. And 94% of patients who had a virtual visit said they’d do it again.
Virtual medical assistants aren’t about replacing doctors or nurses—they’re about extending the reach and resilience of care teams. By taking over repetitive, non-clinical tasks, they allow providers to focus on what matters most: clinical decision-making, patient empathy, and quality outcomes. Think of them as force multipliers, not threats.
Common pushbacks and why they’re outdated
Some of the most frequent concerns around virtual medical assistants simply don’t hold up:
- “Patients won’t trust AI“: Many already use AI in finance, retail, and daily life, and healthcare is next.
- “It’s hard to integrate“: Modern healthcare AI platforms come API-ready and EHR-compatible.
- “We still need human touch“: Exactly. AI frees up staff time so humans can provide it.
What the next 3 years will look like (with or without virtual medical assistants)
With AI: Healthcare becomes more proactive, coordinated, and accessible. Virtual agents help prevent problems rather than just reacting to them.
Without AI: Staff burn out faster, patient expectations go unmet, and operational costs continue to climb. The gap between digital leaders and laggards will widen significantly.
Ready to start? here’s the smart way to pilot
You don’t need to overhaul your entire system. Instead, start small:
- Identify a pain point (e.g., missed appointments, long call center queues)
- Deploy a virtual medical assistant for just that workflow
- Collect metrics: satisfaction scores, response times, workload reduction
- Iterate based on feedback
This phased, measurable approach lets you build confidence and scale responsibly.