
EHR system usage is cited as one of the reasons for an increased burnout rate in healthcare providers. This is problematic, since it could lead to a number of issues, such as a “rise in unprofessional behaviour, a drop in patient satisfaction and a greater chance that a doctor will make a major medical error.”
This is unsettling, since our experience, as well as research, shows that EHR systems are making caregiving easier. So why are healthcare providers unhappy?
According to Dr. John Rogers, MD, one of the prime reasons is the lack of structure in presenting information. In his own words: “too often I pull up a record, either in peer review or another setting, and it’s almost impossible to really get an understanding of the story line. On a daily basis I can’t find the information, particularly nurses’ notes and [other information] that are really valuable to me.”
This is problematic. As we’ve discussed previously, patient history is critical to care giving. Trying to give care without a complete, Uniform Patient Record(UPR), could lead to negative outcomes.
Due to it being mandated technology, most health systems and larger ecosystems have already adopted electronic health record systems. However, that doesn’t mean we can disrespect, and we definitely cannot replace, the experience and knowledge that providers bring to the table. Any true impact that technology will have will first garner the approval (and buy-in) of providers and technology must make practising their profession easier, not contribute to their burnout.
After all, tech can be replaced easily; the care provider, not so much.
Interestingly enough, it doesn’t have to be one or the other. Just a few modifications of the EHR system could help reduce this issue. Cognitive design is “the art and science of bringing harmonic geometry to a conversation.” To put that in layman’s terms and as to how it relates to EHR, cognitive design is used to make tasks simpler.
Healthcare providers have important medical information they need to retain and process in times of need; overloading them by making them have to deal with a cluttered EHR system will detract from their effectiveness. They need an EHR that is simple.
An ideal EHR system is one that makes relevant features and information easily accessible, while eliminating distracting ones. This reduces the amount of data that providers have to process, which will let them worry about more important things, like building patient rapport, diagnosing symptoms properly and focusing on making minimal, if not no, errors.
Let’s dig into a specific example of how cognitive design improves the user experience:
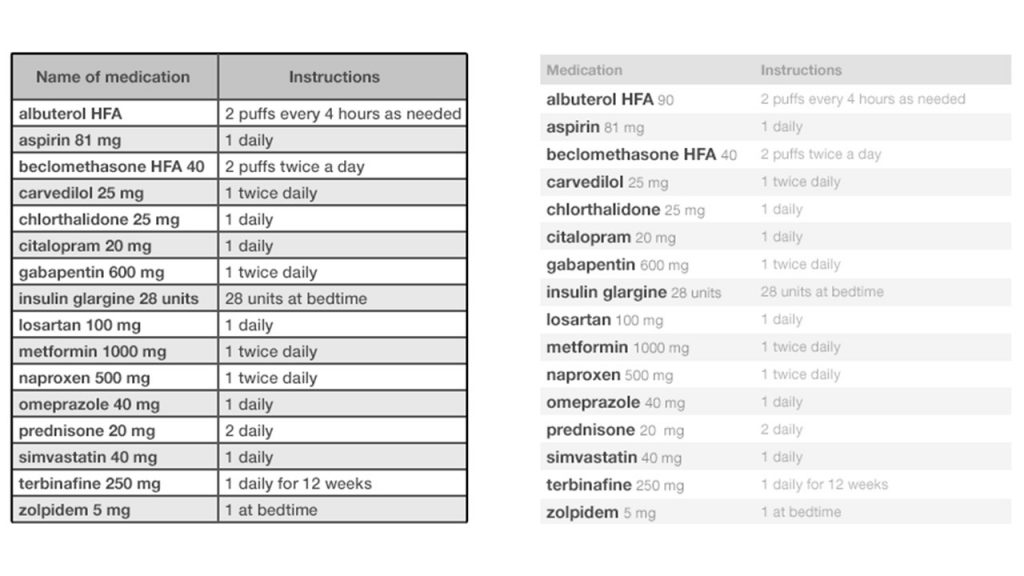
Photo credit to Inspired EHRs Medication List in the first example above, there are too many visual distractions. The frame and instructions draw attention through their dark, bold color and the design detracts from the focus: medication names and dosage. It also looks dated, like something found in a Chemistry textbook from the early 2000’s.
The second image fixes these issues by removing the border, emphasizing the data that is primarily needed and fading the less relevant information. Along with the 3D visualization this gives, it looks fresh and eye-catching.
While the above seems like a small change or nitpicky, it very well could be the difference between a healthcare provider who is happy and easily focused on their work, or a healthcare provider who is unfocused and at risk of making an error.
The healthcare industry is going to continue to rely on our EHR systems and we have to do whatever it takes to reduce, not add to the burnout in an already stressful industry.
